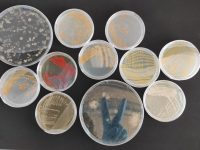
This may come as a surprise, but about 1.5 kg of our body is made up of microbes. Estimates vary, but for every cell in our bodies we harbour at least one microbial cell, around 40 trillion of them overall. The collective genome of our microbiome, the sum of the genetic material of all the microbes that live permanently in our body, is larger than our own by at least an order of magnitude. This means that we have at least ten times more genetic information «for» the life of the microbes in our body than «for» our own. Despite these stupefying facts, since Leeuwenhoek’s description of these «small animalcules» up until barely a decade ago, we have largely ignored these tiny sempiternal passengers of ours.
Fortunately, the advent of modern genetic techniques is radically upturning this situation. For example, we are beginning to understand that the composition of our intestinal microbes (where most of our microbiome reside) is tightly linked to our immune system. Distant relatives to Clostridium difficile, a bacterium that causes acute diarrhoea with potentially fatal consequences, maintain our intestine free from external infections and interact with our immune system to prevent inflammations and maintain a healthy intestinal barrier. Even more exciting, our own immune system seems to «culture» these beneficial bacteria, and it does so at least partly in response to bacterial control, who use it to make themselves a nice and comfy home. As a matter of fact, we suspect that unforeseen changes in our microbiota due to the indiscriminate use of antibiotics and the spread of sugar and fat-rich diets may be responsible for the high incidence of both allergies and autoimmune diseases that plague the most developed human societies in the world.
Apart from a keystone ingredient to a healthy gut, microbiota also seem to communicate with our brains. Either indirectly, by secreting metabolites that influence our immune system, or directly, by secreting neuroactive compounds that act upon our brains. In mice, for example, disrupting the microbiome can alter different cerebral functions to the point of blocking the ability to recognize individuals and causing anxiety and a suite of behaviours akin to those observed in depression and autism. The shocking final twist to this story is that these symptoms almost completely disappear when the gut of sick mice is recolonized with beneficial gut bacteria. The expression «gut feeling» seems to be taking an altogether new and mysterious meaning.
Of course, the story of this relationship only makes sense in the light of evolution. We have coexisted with our microbial partners for several hundred (in some cases thousand) million years, a time we have spent adapting to each other and, together, to the environment we both live in. Recent studies with the Hadza of Tanzania, a group of hunter-gatherers that has inhabited the Rift valley for millennia, indicate their microbiota is much more diverse than our own, and one capable of digesting a much wider range of food sources than we would be able to pass through, and to withstand the almost perpetual presence of different types of intestinal parasites and pathogens that would, quite literally, get us on our knees. This alone gives us an idea of the degree of adaptability and evolutionary importance of our microbiome, for it seems evolution has bounded our destinies much tighter than we could have imagined. The survival of gut microbial crucially depends on this intimate relationship with our bodies, as does our welfare, health and maybe even our sanity. We are entering into a new and exciting biological era: the exploration of our microbial self.