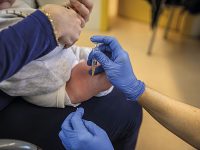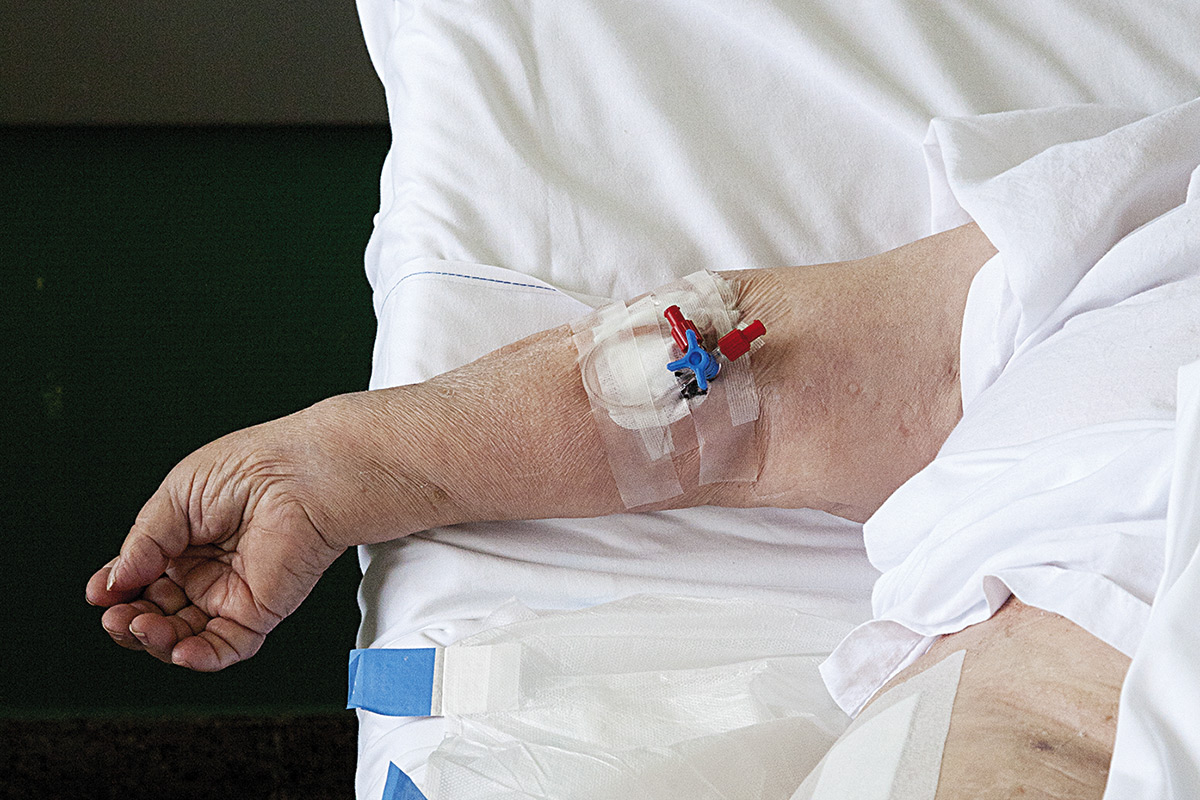
Pain can have far-reaching effects on people’s quality of life. Improper treatment is a serious healthcare issue and an ethical problem of the first degree, directly affecting people and potentially undermining their dignity. The absence of adequate pain assessment and management violates the basic ethical principles of autonomy, welfare, nonmaleficence and justice.
Ethics is a philosophical discipline dealing with moral issues, that is, our behaviour –actions, habits and life in general– from the viewpoint of what is good, dutiful or valuable, qualifying behaviour as good or bad, right or wrong, valuable or devoid of moral value. When it comes to pain, an ethical approximation is also suitable, and when referring to the ethical aspects of pain we are doing nothing more than asking ourselves within this topic area «What is right?» and «What is wrong?». That is, what should and should not be done with respect to this healthcare issue?
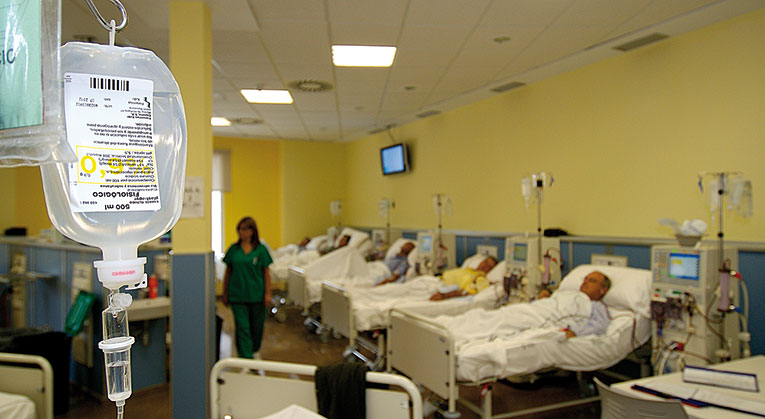
Pain can have far-reaching effects on people’s quality of life, with important consequences in personal, family and social circles. Currently it is a major public health problem. / © De La Ribera University Hospital, Alzira
Pain control and dignity
Pain is an unpleasant experience that affects all human beings at some point in their lives and, despite highly developed knowledge regarding this ailment, today it is still inadequately treated. Pain can have far-reaching effects on people’s quality of life, with important consequences in personal, family and social circles. It is a major public health problem given the large socioeconomic impact it has, due to the consequent use of health services, the loss of productivity in the work ambit and disability subsidies to be paid.
Despite the progress made both in the understanding of mechanisms involved in pain processes and treatment thereof, there is a huge gap between knowledge and practical applications. This is true for both chronic and acute pain. The causes are multiple: culture, attitudes, education, economic capacity and health policies.
Furthermore, there is enough research to support the statement that inadequate pain relief, as well as diminishing the overall quality of the affected patient’s life, also decreases their life expectancy. Although there are situations for which there are no valid therapeutic alternatives at present, unnecessary pain is a serious healthcare problem. This can be defined as persistent pain, due to inadequate treatment or absence of any therapeutic measure, despite availability of effective therapies.
Even today millions of people suffer different types of pain that can be avoided. This lack of consideration for others’ pain by health professionals is an ethical problem of the first degree, directly affecting people and undermining their dignity.
«Pain is an unpleasant experience that affects all human beings at some point in their lives and, despite highly developed knowledge regarding this ailment, today it is still inadequately treated»
Numerous studies, conducted in recent years, indicate that even in cases where pain is treated, the treatment is inadequate or insufficient. B. Ferrell talks about the triple whammy effect: the doctor prescribes quantities below what is necessary, nurses administer less than that prescribed and patients do not report their pain fully.
After many years of neglect, in August 1999, the Joint Commission on Accreditation of Healthcare Organisations (JCAHO) finally included pain control in their standards. The aim was for pain to be considered the fifth vital sign and therefore be monitored in a similar way as body temperature, pulse, blood pressure and breathing.
It is difficult to justify continued suffering of unnecessary pain, without it being considered an act that violates people’s dignity, as might occur with physical or psychological violence. Due to the magnitude of the problem, the International Association for the Study of Pain and the World Health Organisation consider pain relief as a fundamental human right.
Ethical Considerations
Truly ethical attitudes call for solidarity with those who suffer, and encourage us to make all the tools and knowledge available to relieve pain, whether or not they are within reach. If we do not have the necessary skills, we refer the patient to those who have them. Avoiding pain and suffering is the first moral and professional obligation not only of doctors, but also of all professionals involved in patient care.
«There is enough research to support the statement that inadequate pain relief, as well as diminishing the overall quality of the affected patient’s life, also decreases their life expectancy»
For most people, the concept of a «dignified death» is associated to dying without pain, surrounded by family and without excessive intervention. The intensity and bitterness of the current debate on the right to a dignified death would diminish considerably if society, clinicians and health policymakers paid more attention to ways of mitigating the patient’s pain and suffering. They should grant the patient’s values, well-being and wishes with the respect and esteem they deserve, and should view someone’s death with more compassion and forbearance. A good death is difficult to define but easy to detect, and awakens a deep sense of awe and humility before the well-being and dignity of human beings.
The absence of adequate pain relief seems to be a remnant of Cartesian dualism, which dichotomised the physical and the mental, and where the body is taken clinically as the place for physiological determination. Although human beings exist through their body, the body is not only the psychophysical place where disease acts, but the person’s dimension where suffering is experienced and the person as a whole is affected. The corporeal is not something a person has but something that the person is.
Suffering involves the individual’s values and well-being, as well as the underlying physical causes. Thus, in addressing pain the psychological, social and spiritual aspects of analgesic therapy are not ornaments but essential components of good pain management. This dichotomy has led physicians to assume responsibility solely for the treatment of physical and biological aspects of disease, while they leave suffering to be treated by psychologists, priests and social workers.
Proper pain relief is a priority in the care of all patients, and is deeply rooted in the origins of the medical profession. Physicians have the responsibility to treat both the patient and the person, which means they have to assess and treat the pain and suffering of each and every one of their patients. Failure to do so implies an unfulfilled responsibility, that is, they can be held accountable to patients and to society as a whole.
The welfare state which has been achieved, in European countries especially, promotes the worship of beauty, of what is young, the desperate search for happiness, understood as a kind of permanent nirvana of continuous and inexhaustible pleasure, where there is no place for the sick, the weak, the bad or the ugly. In this context, however, we should not be tempted to identify the rejection of unnecessary pain and unnecessary suffering with a hedonistic attitude.
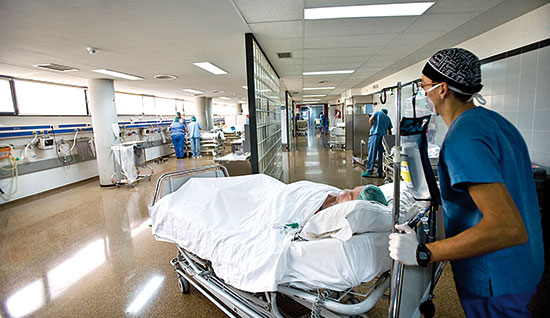
Truly ethical attitudes call for solidarity with those who suffer, and encourage us to make all the tools and knowledge available to relieve pain. / © De La Ribera University Hospital, Alzira
Principlism and ethical analysis
With the birth of bioethics, a number of models or ethical paradigms have been put forward to approach the new discipline. The most widespread and popular in the biomedical field is principlism. Its founders, Beauchamp and Childress, took the famous principles of the Belmont Report –true foundational letter of bioethics– as the starting point of principlism.
This model advocates that medical practice, and in general all relationships between healthcare workers and patients, should be governed according to four moral principles: beneficence, nonmaleficence, respect for persons (autonomy) and justice. These four principles would, prima facie, be principles to be respected equally, but when in conflict the hierarchy between them should be established for each individual case. The absence of adequate pain assessment and management violates these basic ethical principles.
Respect for a person implies two ethical convictions: that everyone should be treated as an autonomous entity and that people with diminished autonomy are entitled to protection.
In the present case, to respect patient autonomy is, firstly, to involve the patient in their treatment, to believe in the pain they manifest, inform them of the alternatives available to treat their pain and design a pain-relief plan with them. Properly informing the patient and respecting their preferences helps to reduce anxiety caused by pain and favours speedy recovery.
By contrast, we know pain destroys a person and considerably reduces their autonomy, making them more dependent; furthermore, inadequate pain relief helps perpetuate or even leads to a decline in autonomy. The principle of beneficence requires us to seek what is good for the patient above all. Allowing a patient to suffer pain, without providing the necessary means to prevent it, openly violates the principle of beneficence. Moreover, pain itself produces its own morbidity while adequate pain relief improves prognosis and facilitates recovery.
The principle of nonmaleficence, traditionally associated with primum non nocere, requires us to avoid inflicting harm on the patient, minimising the risks of intervention. There are situations where it is impossible to avoid trauma to the patient, given the invasiveness of surgery and certain diagnostic tests. In these cases, failure to use all means necessary to prevent or reduce pain and trauma of surgery as far as possible, is to act in such a way as to inflict pain and suffering. This is a harmful action that could be avoided and is thus considered wrong. Ignorance can never be used as an excuse or as defence, and the lack of proper training or knowledge leads directly to malpractice.
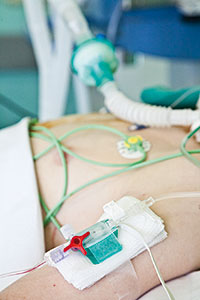
© F. Morant
Both physicians and other professionals working in patient care have the responsibility to be appropriately qualified and to posses up-to-date knowledge on drugs and other techniques that benefit patients. If, for some reason, this is not possible then they have the responsibility and ethical duty to consult professionals who are properly trained to handle pain. Defending ignorance is to violate the goals of medicine and to breach doctors’ basic duty towards their patients. Gomez and Ojeda tell us: «Inadequate pain relief is the most outrageous and persistent medical malpractice».
Failure to use available resources to alleviate pain should be considered an act of professional negligence, as it causes unjustified harm to the sufferer. Even before any ethical analysis, it is necessary to determine the technical correctness of the procedure.
The principle of nonmaleficence also requires us to weigh the benefit versus risk of each analgesic intervention, and to know the side-effects of drugs and analgesic techniques. It obliges us to choose those with better therapeutic and safety profiles, taking into account the patient’s clinical situation and characteristics. Health professionals, as moral agents, have an ethical responsibility to treat our patients so as to maximise the benefits and minimise the harm.
«Truly ethical attitudes call for solidarity with those who suffer, and encourage us to make all the tools and knowledge available to relieve pain»
The principle of justice demands equality in the medical treatment received by each patient, and this is violated when some receive proper pain relief but others do not, depending on the professionals or institutions they are assisted by. Justice dictates that similar medical conditions should be treated similarly. All patients are entitled to have their pain assessed and treated adequately. Ignorance or the unequal distribution of healthcare resources is no excuse or defence in a society that guarantees the universality and equity in access to healthcare.
Finally, with respect to resource availability and distribution, although there are many high-cost techniques, analgesic treatment is –generally speaking– easily affordable. Indeed, there is a wide range of powerful low-cost drugs available and analgesic therapy is an essential component of good pain management.
Beachamp, T. L. i J. F. Childress, 1999. Principios de ética biomédica. Masson. Barcelona.
Clark, P., 2002. «Ethical Implications of Pain Management. Can A Formalized Policy Help?» Health Progress, July-August: 19-28.
Gómez Sancho, M. i M. Ojeda Martín, 1997. «El problema del dolor. Historia y análisis de un escándalo». Medicina Paliativa, 4: 20-34.
Macpherson, C., 2009. «Undertreating Pain Violates Ethical Principles». Journal of Medical Ethics, 35: 603-606.
Rich, B., 2000. «An Ethical Analysis of the Barriers to Effective Pain Management». Cambridge Quartely of Healthcare Ethics, 9: 54-70.
Soler Company, E. i M. C. Montaner Abasolo, 2003-2004. «Consideraciones bioéticas en el tratamiento del dolor». Persona y Bioética, 20-21: 49-63.
Torres, L. M., 2005. «El tratamiento del dolor como un derecho de todos». Revista de la Sociedad Española del Dolor, 12: 399-400.