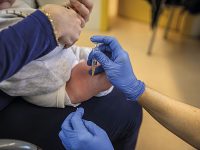
Pain is one of the symptoms for which patients seek medical treatment most. It affects 12% of the population and is considered severe in one third of these cases. This article reviews the different types of pain, both acute and chronic, and new pain-management treatments. Nowadays, we have multiple options available, which offer sufferers the possibility of a better quality of life.
According to a recent European Union survey, pain is one of the main reasons why patients consult their GP. Nonetheless, pain is still underestimated and under-treated by both health professionals and patients alike.
In Spain, endurance of suffering is part of our Mediterranean culture, as is character building through pain. This, together with very limited public resources for pain management, leads to a situation where when patients suffering pain, sometimes excruciating pain, go to specialised treatment units, they find they are totally overrun.
«Pain is one of the main reasons why patients consult their doctor. Nonetheless, pain is still underestimated by both health professionals and patients alike»
Pain in Spain
The Pain in Europe survey, the largest ever conducted on chronic pain and including sixteen European countries in 2005, revealed that in Spain 12% of respondents stated they suffered from chronic pain, and 31% of these were in constant pain. The average duration was found to be 9.1 years, being more frequent in women (12.4%) than men (6.4%). Furthermore, 3% of patients in pain had been forced to stay in bed more than half a day. The most frequent pain is in the back, joints and bones. Almost one in three respondents had taken a painkiller of some kind in the fifteen days preceding the survey.
The traditional classification of pain, which is still used today, distinguishes four different types of pain: chronic non-cancer pain, chronic cancer pain, acute postoperative pain and chronic postoperative pain.
Chronic non-cancer pain persists more than three months or even six months, and on a daily basis or, at least, no less than five days a week. Its intensity is moderate –at least– and can impair the functional capacity of sufferers. Regarding Spain, the Pain in Europe survey highlights that this type of pain is more common in women (52%) than in men (48%) and 22% of respondents categorised it as severe and 18% as unbearable.
«In Spain, endurance of suffering is part of our Mediterranean culture, as is character building through pain»
Within this category, the most frequent is knee pain (28%) followed by back pain (23%) with 20% of the patients taking five to ten years to achieve optimal pain control. This type of pain can be treated effectively with analgesics and adjuvants (antidepressants, neuroleptics, steroids…), although a considerable number of patients require interventional techniques, meaning oral medication can be withdrawn.
Another category is chronic cancer pain. This is long-lasting pain within the context of cancer, which can be the direct or indirect cause of pain (immobilization, treatment, intercurrent disease…) and is one of the symptoms most feared by cancer patients. Opioid analgesics are the main treatment but may be limited due to their side effects, which sometimes necessitate the application of interventional techniques.
Cancer pain affects seven out of every ten patients moderately to severely, and one in four does not receive any analgesic treatment. The EPIC survey on cancer pain in Europe, published in 2009, reveals that pain is the primary reason why patients seek medical advice. What is more, 96% of patients had experienced pain during the previous month.
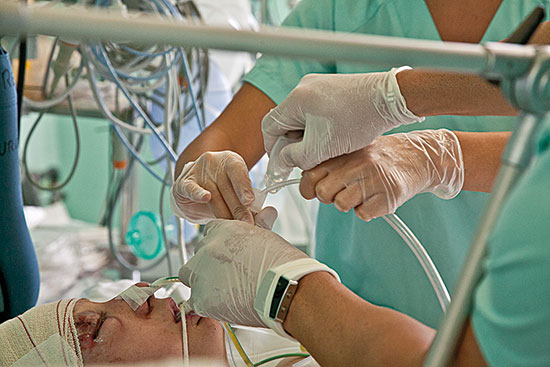
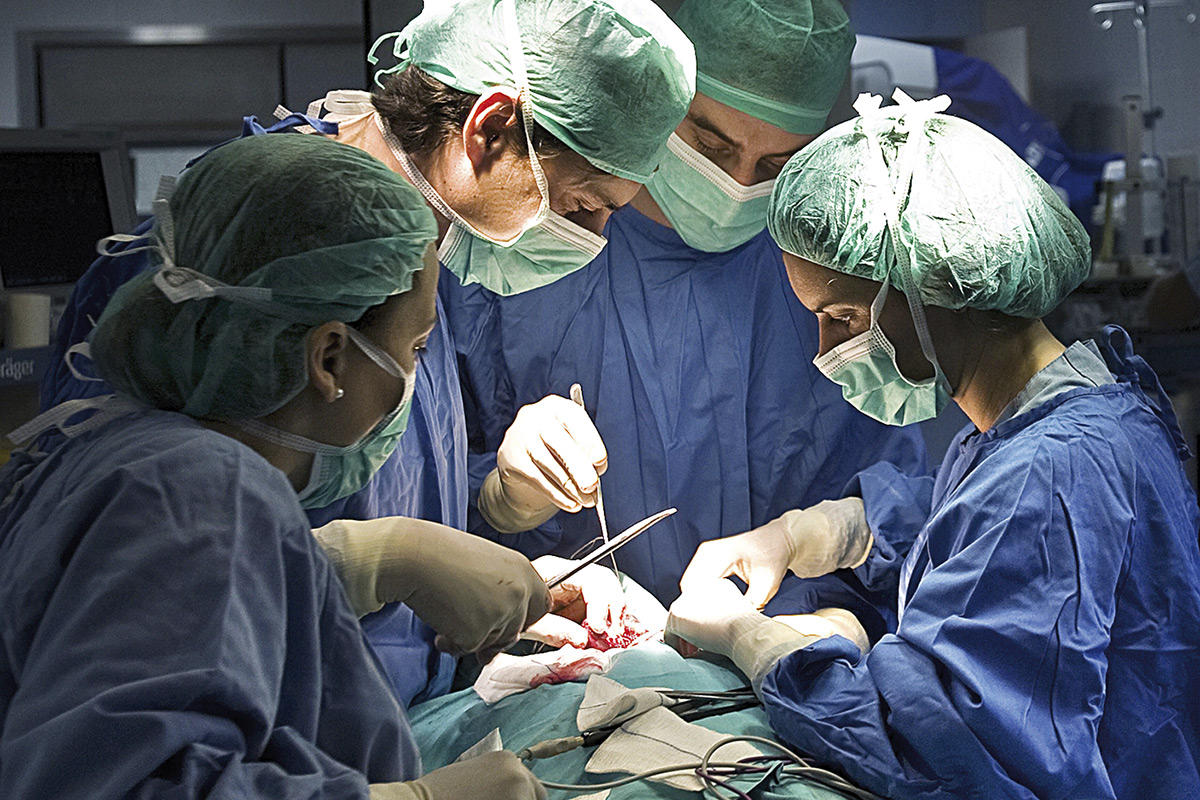
About 85% of hospitalized patients undergoing major surgery suffer postoperative pain during hospital confinement. It is important to control this pain both for patient wellbeing and to facilitate recovery. / © F. Morant
Next, we differentiate acute postoperative pain, which is the type experienced after a surgical procedure, and has a limited duration unless it becomes chronic. As it is foreseeable in most cases, it can be treated even before it appears. Around 85% of hospitalised patients undergoing major surgery experience it at some point during their hospital confinement. The percentages vary significantly, depending on the type of surgery and the analgesic protocol.
Pain management is essential not only for the patient’s comfort but it can also mean better recovery and speedier discharge from hospital.
Finally, chronic postoperative pain is the type of pain that occurs after surgery and lasts longer than two months. Any other aetiology should be ruled out and it should not be a continuation of a preoperative problem.
Certain types of surgery are more likely to lead to chronic pain, including: thoracotomy (20-80%), the inguinal herniorrhaphy (4-53%) and hysterectomy (5-32%). There is a genetic component that may favour it, but there are other factors such as preoperative anxiety, female gender or previous interventions in the same area.
Treating postoperative pain
Pain can be controlled by administering analgesics systemically (orally or intravenously) or by using regional techniques. Regional techniques enable analgesia to be limited to the anatomical area subjected to surgery, thus having limited side effects as it decreases the risks associated with drug administration (nausea, vomiting, constipation, renal failure, thrombocytopenia…).
To achieve full postoperative recovery and adequate pain relief, a rehabilitation program must take into account other factors that may hamper recovery, such as hypothermia, immobilization, or the irrational use of catheters, hypoxemia and the like.
«Nowadays we are able to offer most patients a better quality of life. As long as techniques are applied appropriately, pain becomes tolerable, irrespective of its origin»
Pain relief
Depending on the location of surgery, the exact nerve territory affected must be considered to achieve the best possible pain relief. According to the location of the analgesic technique, differentiation is made between neuraxial techniques (focused on blocking the pain impulse in the spinal cord), which include epidural and subarachnoid and peripheral nerve blocking techniques. The difference between epidural and subarachnoid neuraxial blockade lies in the place where the local anaesthetic or analgesic is administered. In the former, it is deposited outside the duramater and the latter inside the subarachnoid space, mixing with cerebrospinal fluid. Peripheral nerve blocks do not block the stimuli at the spinal level but directly target the nerve or set of nerves (nerve plexus) and the analgesic or local anaesthetic is deposited nearby.
The success of any continuous analgesic technique lies in suitable recommendations based on the surgical procedure, proper positioning of the catheter, the right choice of drugs to be infused, with beneficial association of local anaesthetics and opioids, and an appropriate pain management system.
Painkillers
Analgesics (anti-inflammatories, opioids, local anaesthetics…) can be administered as a bolus (administering an amount of the drug directly into a particular zone), by continuous infusion or in the patient-controlled analgesic mode intravenously, as epidural or perineural.
The administration of bolus at regular intervals implies a lower overall cost; however, it does not meet the analgesic requirements of most patients adequately. This is because not all patients feel the same intensity of pain after surgery, and bouts of pain may arise between doses, when pain relief is insufficient for some patients.
Continuous infusion allows for better pain relief but does not adequately cover the peaks of pain the patient may experience.
Meanwhile, patient-controlled analgesia, where the patient manages the level of analgesia required, provides high quality treatment with greater satisfaction, especially when continuous infusion is associated with bolus on demand. However, this system is more costly and requires greater participation of the patient and enough clear thinking to understand how the system works.
Neuraxial techniques
Neuraxial techniques are commonly used by anaesthesiologists, primarily because of their effectiveness during surgery. The epidural technique is most often used postoperatively, providing quality pain relief with minimal side effects and remains the most effective analgesic method after laparotomy in digestive surgery. In thoracic surgery, epidural administration of local anaesthetics with opiates is the recommended technique, showing a similar analgesic efficacy as paravertebral block and better than systemic analgesics or intercostal infiltration.
The benefits of epidural with local anaesthetics are particularly clear when treating pain within 72 hours of surgery when compared to patient-controlled intravenous analgesia. This system improves the endocrine-metabolic impact of surgery and provides significant advantages in patients at high risk of cardiac or respiratory disease, and possibly reduces the likelihood of chronic pain.
«Depending on the location of surgery, the exact nerve territory affected must be considered to achieve the best possible pain relief»
Peripheral techniques
Single-shot peripheral nerve blocks provide quality postoperative pain relief over a period of up to 24-36 hours, even using new-generation local anaesthetics.
Since they were first described by Ansboro in 1946, continuous nerve block techniques by catheter occupy a prominent place in bibliography dealing with pain management and regional anaesthesia. The use of catheters for postoperative pain relief has extended the analgesic effects beyond the surgical operation itself, and –along with quality analgesia– has allowed early rehabilitation and speedy patient discharge.
The continuous peripheral techniques most commonly used for postoperative pain relief are the interscalene block for shoulder surgery, infraclavicular block for elbow surgery, the femoral nerve block for knee surgery and sciatic block for foot surgery.
Dealing with chronic pain
Analgesic options for treating chronic pain have changed significantly in recent years, with new routes of administration, new forms of drug delivery, plus invasive pain-relief techniques that provide better pain control and analgesic efficacy.
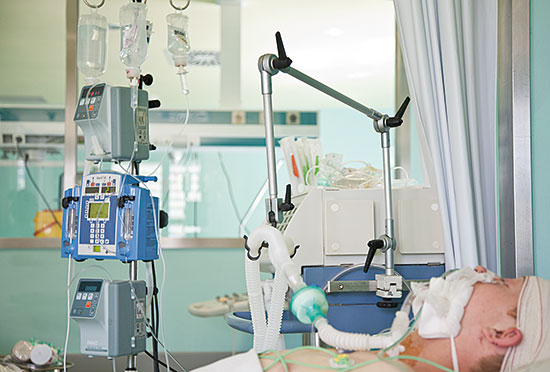
There are several pain management techniques. Continuous infusion allows for better pain control, but does not adequately cover the peaks of pain the patient may experience. / © F. Morant
The pathologies most frequently treated in chronic pain units are: back pain (spinal stenosis, degenerative spondylarthrosis, pain after failed back surgery, post-laminectomy syndrome), neuralgia (trigeminal, secondary to herpes zoster…), complex regional pain (types I and II), traumatic injuries of nerves, functional disturbances (headaches, myalgia) or postoperative neuropathies (especially after thoracotomy, herniorrhaphy or vascular surgery).
The use of devices, attached to the skin, through which the drug can diffuse, has been a major step forward in chronic pain management. The latest patches contain a reservoir of opioids in gel form, as well as a diffusion-limiting membrane which lets a fairly steady flow through for 48-72 hours. This procedure allows for greater patient comfort by reducing the multiple daily doses of painkillers.
In addition, new analgesic administration formats allow patients to quickly and adequately control their pain, which is especially useful in cases of cancer breakthrough pain, in which relief is achieved within a few minutes and lasts a predictable time.
On the other hand, regarding interventional techniques in chronic pain management, multiple invasive techniques can be used in patients with chronic pain, from simple nerve blocks and infiltration to more sophisticated techniques that include radio frequency lesioning, spinal infusion or spinal cord stimulation.
All these techniques may be used on different targets. However, sometimes it is essential to verify or perform diagnoses before using the more sophisticated techniques as the source of the pain may not be clear and the exact source of pain must be located first. Blocking can be employed to temporarily reduce pain or to allow patients to carry out rehabilitation which they would not be able to if they were in pain.
«Pain is one of the main symptoms causing patients to seek medical care. Nowadays we have both the pharmacological tools and interventional techniques to tackle it together»
These techniques are usually performed in sterile rooms –preferably surgical areas– and to carry them out, different localization support methods are required. Practitioners may use nerve stimulation, ultrasonography, computed tomography and even magnetic resonance imaging, all with the sole aim of reaching the target area more accurately.
Radio frequency uses electrical currents exceeding 500,000 Hz to produce well-defined lesions, which can be predicted by controlling electrical parameters, temperature and electrode measurement. The therapeutic effect is achieved by the heat and electromagnetic changes generated. Conventional radiofrequency can also be used, typically reaching temperatures of 80 °C, or pulsed radiofrequency, which reaches temperatures of 42-45 °C with a pulsed rather than a continuous current.
Radiofrequency is mainly recommended for spinal pains but is also being applied to peripheral joints (shoulder, knee…), peripheral nerves (greater occipital nerve, sural nerve…), and the like.
Spinal cord stimulation is a neuromodulation technique that modulates pain transmission using electrodes implanted in the epidural space. It is mainly used to treat neuropathic and ischemic pain and can also be used for chest pain (angina).
So, we can see from this review of the main techniques and approaches to controlling acute and chronic pain that, nowadays, we are able to offer most patients a better quality of life. As long as techniques are applied appropriately, pain becomes tolerable, irrespective of its origin.
In the eighties, the view that the French health authorities held on the treatment of pain changed totally. The reason was that a relative of the Minister of Health at the time was suffering from a pain that was difficult to control, and could not find quality care at one of the most difficult times in life. From that moment on, an active policy began. Pain-management and palliative-care units were set up, training programmes were run for health professionals as well as public awareness campaigns and research into new therapies was promoted. All this led to an improvement in the quality of life for French citizens.
Pain is one of the main symptoms causing patients to seek medical care. Nowadays we have both the pharmacological tools and interventional techniques to tackle it together and, so doing, we can improve the quality of life of patients suffering pain.
Aliaga, L. et al., 2009. Tratamiento del dolor. Teoría y práctica. 3rd edition. Publicaciones Permanyer. Barcelona.
Aliaga, L. et al., 2006. Anestesia regional Hoy. 3rd edition. Publicaciones Permanyer. Barcelona.
Breivik, H. et al., 2006. «Survey of Chronic Pain in Europe: Prevalence, Impact on Daily Life, and Treatment». European Journal of Pain, 10: 287-333.
Breivik, H. et al., 2009 «Cancer-related Pain: a Pan-European Survey of Prevalence, Treatment, and Patient Attitudes». Annals of Oncology, 20: 1420–1433.
Català, E. et al., 2002. «Prevalence of Pain in the Spanish Population: Telephone Survey in 5,000 Homes». European Journal of Pain, 6: 133-140.
Lee, A. et al., 2007. «Economic Evaluations of Acute Pain Service Programs: a Systematic Review». The Clinical Journal of Pain, 23: 726-733.
Macrae, W. A., 2001. «Chronic Pain After Surgery». British Journal of Anaesthesia, 87: 88-98.
McMahon, S. B. & M. Koltzenburg, 2006. Wall & Melzack. Tratado del dolor. Elsevier. Madrid.
Vallano, A. et al., 2007. «Estudio multicéntrico de la evaluación del dolor
en el medio hospitalario». Revista Española Anestesiología, Reanimación y Terapéutica del Dolor, 54: 140-146.