A diseased ecosystem
Tackling antibotic resistance from a global perspective
DOI: 10.7203/metode.78.2627

Man’s production of antibiotics has led to disease in microbial ecosystems on a planetary scale. The most immediate impact for man is the intractability of infections. To tackle this we must improve our understanding of this phenomenon, and develop intervention strategies employing novel conceptual, analytical and technological methods.
Keywords: eco-evo strategies, global medicine, antibiotic resistance, multi-hierarchical analysis.
To treat human health and prevent disease, public health systems require epidemiological information on the scale (incidence and prevalence) of the phenomenon under study, enabling possible causal associations to be defined. It is becoming increasingly clear that human health is dependent on global health as a whole; in other words, the health of the environment of which man is a part. Accordingly, efforts to control the forces that adversely affect human health should include not only the analysis of human diseases, but also of all other animals (one-health perspective), plant diseases and of our massive micro-biosphere. The latter is the set of microbes covering our planet, which know no bounds, and whose existence and balance greatly depends on the existence of beings which, somewhat lacking objectivity, we call «higher».
A planetary medicine
Human health depends on our planet’s health. Of course, the biological success of Homo sapiens has profoundly changed the Earth, to such an extent it is conceivable to say that man has started a new geological epoch, the Anthropocene, in which nature has been modified and stressed by human action. This anthropogenic activity is determining the future of biological evolution on our planet. The problem that concerns us here, bacterial resistance to antibiotics, is a good example to illustrate how anthropogenic modification of the environment has deleterious effects for the human species.
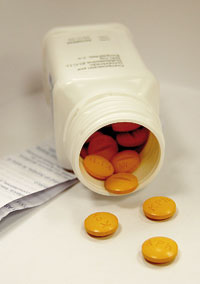
Industrial production of antibiotics has created a serious «global antibiotic pollution». One of our planetary diseases is due to mass production of antibiotics and their release into the environment. / Agencia SINC
Probably we will need to establish real «global medicine». The idea is based on considering the entire planet as a «subject» that requires medical attention. The long refined medical methodology, intended for individual patient care, must be scaled up to planetary size, starting off by defining the signs and symptoms of planetary diseases. We must also study their pathogenesis and pathophysiology, assess their potential to spread worldwide, establish diagnostic methods ranging from imaging technologies to advanced molecular identification, and thus endeavour to make ecological and evolutionary predictions. This would be followed by specific interventions, including surgery, developing treatments and future eco-evo1 (Baquero et al., 2011), containment and isolation methods, or even the application of intensive care and preventive measures. As stated above, the problem of antibiotic resistance is a model-problem for future planetary medicine. No doubt, the planet is «sick from antibiotic resistance» and this disease, which affects the micro-biosphere, means many humans are colonized by abnormal bacterial communities, often antibiotic-resistant microorganisms.
In order to accurately diagnose diseases in the planet’s micro-biosphere, we must improve the criteria and sensitivity of methods used to measure microbial diversity. Changes in diversity should be one of the key-analyses used to detect disease symptoms and progression. Undoubtedly, to achieve this goal we must first reconsider bacterial biological units. We cannot continue to use the old Linnaean classification of «microbial species». Of course we cannot seriously maintain that there are 20,000 «well defined» bacterial species, if we have identified 300,000 plant species and 10 million arthropods. There must be at least one billion bacterial species, according to some estimates based on mathematical extrapolation of metagenomic studies. Obviously, we have to improve our culture techniques; the recent proposal of «bacterial culturomics» (natural sample inoculums in multiple media) will probably improve our analytical skills. And naturally, we must redefine the concept of bacterial species.
Antibiotic pollution
Man has managed to produce antimicrobial substances to fend off infectious diseases which, either on an individual level or under the terror of great epidemics, have plagued our species. All modern medicine has developed under the «protective umbrella» of antibiotics. Without antibiotics, a huge proportion of our elderly and our newborns (with lower defences against infection) would die of infections. Without antibiotics, intensive-care units are inconceivable, cancer therapy, care of premature infants, complex surgeries or organ transplants. The problem is that industrial production of antibiotics has created remarkable «global antibiotic pollution». As one of the many planetary diseases, this one is due to the effect of mass production of antibiotics and their release into the environment.
Industrial production of antibiotics is a paradigmatic example of the type of anthropogenic substances that exert a powerful effect on the micro-biosphere. Indeed, with the annual production of antibiotic drugs, one could cover the Earth’s surface with a layer capable of removing bacteria. Antibiotics not only eliminate trillions of bacteria non-specifically, but this deletion can promote the selection of resistant organisms. The fact antibiotic pollution of our planet leads to the selection of resistant bacteria (which are potentially pathogenic to humans and thus able to cause untreatable infections) is of great importance. However, rather more significant are effects of a more «ecological» nature, which could result from the elimination of natural populations and their replacement by others. Industrial antibiotics are modifying bacteria ecogenetics and accelerating the development of the micro-biosphere, by increasing selective forces and promoting microorganisms’ capacity for variation (mutation, recombination, transposition, modularization, gene transfer) (Galán et al., 2013).
«Man has started a new geological epoch, the anthropocene, in which nature has been stressed and altered by human action»
It is essential to understand that most antibiotics are natural substances. In reality, there must be a huge number (hundreds of thousands?) of natural antibiotics, and only a tiny fraction (less than a hundred) have been industrially produced and used in human and veterinary medicine. What is the natural function of antibiotics? Antibiotics are substances that mediate intercellular communications, «organizer» substances of the life cycles and homeostasis of microbial populations and communities. The role of antibiotics in nature is not necessarily, as it might seem at first glance, to intervene as a weapon in the «war between bacteria». Firstly, their inhibitory effect on the growth of other microorganisms has a defensive rather than offensive function. Secondly, elimination of other bacteria is not the aim of this inhibitory effect, but only the prevention of excessive overgrowth of microorganisms in an integrated ecosystem. The spreading of the antibiotics secreted by the antibioticproducing bacteria ensures that the bacterium is surrounded by an «exclusive zone». Within this zone, potentially competing bacteria come up against low antibiotic concentrations, which, although insufficient to eliminate them, are enough to reduce their growth rate and avoid overpopulation. These inhibition phenomena are frequently reciprocal and multilateral, ensuring diversity and balance of the whole. In this respect, bacteria are profoundly «democratic», or at least, are fully compatible with –and a perfect example of– statements by Thomas Hobbes (1588-1679) on how natural laws curb each individual’s liberty to dominate in order to ensure common existence, and, in short, biological existence itself. Antibiotics are a part of the complex network of intercellular and interpopulation signals that maintain differentiation and diversity in the micro-biosphere (Linares et al., 2006). Therefore, they act as «signal molecules», like hormones integrating the operation of complex systems. As with the majority of signals, their physiological «signalling» concentration is probably very low.
In contrast to this natural scenario, anthropogenic production of antibiotics exceeds the production of intercellular «signals» on an unimaginable scale, all of which are released into the micro-biosphere. The high density of signals produces a high level of indecipherable «noise», with deleterious effects on the informational networks of biological systems and a host of ecological and evolutionary consequences we are far from being able to decipher.
The fight against pathogenic bacteria: A global problem
Of course, the immediate and conceivable danger of releasing large amounts of industrial antibiotics into the environment (including treated individuals) is the development of resistant organisms within pathogenic bacterial populations, leading to intractable infections. As Stuart Lèvy said in his famous book The Antibiotic Paradox, our misuse of antibiotics is destroying their curative powers. In truth, the problem of antibiotic resistance has reached a point of no return. For a long time –too long– «proper use of antibiotics» has been postulated, in basic terms: less use, with better detection of cases where treatment is really necessary, should lead to a reduction in resistance phenomena. This would be the result of a lower selective effect, and it has been assumed that resistant bacteria pay a certain «biological cost» to maintain this new function, so in the absence of antibiotics, sensitive bacteria would benefit and eventually prevail. It is true that on the individual, hospital, geographical or regional scale, resistance increases in parallel to antibiotic consumption. However, widespread antibiotic pollution has led to a true planetary invasion of resistant bacteria. As Carl Sagan said in his novel Contact, «The boundaries are arbitrary. The planet is real», and thus, in regions with better «antibiotic policy» we can already witness the invasion of bacteria with antimicrobial resistance from external sources.

The misuse of antibiotics in places where large masses of human and animal populations live in sub-optimal sanitary conditions can have global consequences. The bacterium Staphylococcus aureus was «human» in China for many years, passed on to pigs, actively transmitted in farms, adapted to animals and reduced its pathogenicity towards humans. However, in the process it acquired the genetic mechanisms of antimicrobial resistance. In Europe, the resistant clone of this bacterium, CC398, has again infected humans. / Carl Jones
Eastern countries, increasingly interconnected with the West, harbour large masses of human and animal populations, with sub-optimal healthcare and serious deficiencies in environmental health. These factors coupled to increasing growth and development lead to a high degree of antimicrobial use. The result is a «time bomb» or «reactor» where the evolution of antimicrobial resistance is accelerating. There are two good examples refl ecting this situation. The first is the unexpected appearance in Holland of human cases of Staphylococcus aureus resistant to methicillin, and thus to all beta-lactam antibiotics. Molecular studies have shown that S. aureus CC398, the bacterial clone responsible for this infection, reaches Europe through animals of Chinese origin, mainly pigs. This bacterium was «human» in China for many years, passed onto pigs and actively transmitted on farms. There it adapted to these animals and reduced its human pathogenicity, but in the process acquired the genetic mechanisms of antimicrobial resistance. In Europe, the resistant clone CC398 has again been able to infect humans. The second example relates to the emergence in Europe (Sweden and the UK) of strains of Enterobacteriaceae with a new multi-resistant enzyme to beta-lactams, the New Delhi metallo-beta-lactamase (NDM), originating from «importation» by a human carrier from New Delhi, India. In fact studies show that the strain is widespread in this region of India, where it probably emerged. In Europe, a secondary spreading of this strain has occurred, also reaching Spain.
Evolutionary keys
What are the evolutionary keys to this planetary invasion of antibiotic resistant bacteria? What can we do to control this situation? The first evolutionary key is the massive industrial production of antimicrobial drugs, their widespread use in medicine, veterinary medicine and agriculture, and consequent release into the environment. As we have seen, the most predictable consequence is the selection of resistant populations, but also the acceleration of bacterial variation and the distortion of the signalling system that regulates micro-biosphere homeostasis. It would be necessary to regulate not only proper use, but also biodegradation (biodegradable antibiotics) or at least the confinement and treatment of waste containing antibiotics.
The second evolutionary key is the interaction between human and animal-colonizing and/or pathogenic bacteria with other microorganisms in the environment. Environmental bacteria (in soil, particularly in the rhizosphere, and water, especially in sediments) contain a complete repertoire of resistance genes (the environmental resistome), which can be transferred by mobile genetic elements to bacteria that are hazardous for public health. Bacteria from human and animal origin (imagine sewage from hospitals and farms) are spreading into the environment with few limitations. They are contaminating ecosystems with resistance genes amplified by anthropogenic action, and may in turn receive new genes from environmental bacteria. The density of interactions is huge in overpopulated countries with low sanitary levels. Indeed, it is perplexing that epidemiologists and health specialists have not seriously proposed the need to prevent contact between human-animal bacteria and environmental bacteria (Baquero et al., 2008). We are in urgent need of sterilization technology for our waste (sewage) before it is released to the environment, both on the industrial (e.g. waste water treatment facilities for hospitals) and household level, especially in regions with low levels of sanitation (e.g., mini-septic tanks).
«The most immediate and visible danger of releasing high quantities of industrial antibiotics into the environment is the evolution of resistant pathogenic bacteria»
The third evolutionary key is the global dissemination of high-risk bacterial clones, which circulate antibiotic resistance on a global level, and spread it to other bacteria. These clones probably circulate on what Mark Ragan described as «highways of gene sharing», and widespread circulation ensures the progressive recruitment of new genes and the development of multiresistant bacteria. We must improve our technology with rapid techniques for detecting these high-risk clones in people, animals and the environment, and identify the «highways» along which they travel around the planet. We must improve our ability to eliminate these dangerous clones, with clone-directed therapy or by applying specific vaccine strategies. There are precedents for the potential success of these interventions against resistant clones, such as Streptococcus pneumoniae or Haemophilus influenzae vaccination.
The fourth evolutionary key lies in that evolutionary change of antibiotic resistance develops within a complex multi-hierarchical system. Resistance genes, genetic platforms in which they are located, mobile genetic elements (able to move from cell to cell) in which the platforms are inserted, the bacterial cells into which the mobile elements are inserted, the clonal complexes these cells belong to, microbial species and communities, ecosystems, are all the different evolutionary units embedded in each other, forming a multilevel introgressive structure (Bapteste et al., 2012). In fact, we should develop an integrated multi-hierarchy epidemiology, to perform studies of population biology on each independent evolutionary unit, and induce the effects of changes in the various elements forming the complex system (Baquero et al., 2013). Knowing this information, in the future it will be possible to make true eco-evo interventions, including administration of a «drug» to cure certain ecosystems resistance, like the human microbiome for example (Baquero et al., 2011).
In summary, combined ecological and evolutionary knowledge will be needed in the near future to understand and correct major public-health problems. A global health problem that must be addressed is the micro-biosphere’s exposure to massive amounts of antibiotics, whose immediate consequence is antibiotic resistance in bacteria that infect humans and animals.
1. Eco-evo, short for «Ecology and Evolution» refers to a biological approach that considers the possibility of integrate study and action in ecology (environmental cues) and evolution (heritable modifi cation of organisms as adaptation to these cues). (Go back)
REFERENCES
Bapteste, E. et al., 2012. «Evolutionary Analyses of Non-genealogical Bonds Produced by Introgressive Descent». PNAS, 109(45): 18.266-18.272. DOI: <10.1073/pnas.1206541109>.
Baquero, F.; Coque, T. M. and F. de la Cruz, 2011. «Ecology and Evolution as Targets: the Need for Novel Eco-evo Drugs and Strategies to Fight Antibiotic Resistance». Antimicrob Agents Chemother, 55(8): 3.649-3.660. DOI: <10.1128/AAC.00013-11>.
Baquero, F.; Martínez, J. L. and R. Cantón, 2008. «Antibiotics and Antibiotic Resistance in Water Environments». Current Opinion in Biotechnology, 19: 260-265. DOI: <10.1016/j.copbio.2008.05.006>.
Baquero, F.; Tedim, A. P. and T. M. Coque, 2013. «Antibiotic Resistance Shaping Multilevel Population Biology of Bacteria». Frontiers in Antimicrobials, Resistance and Chemotherapy. Prepublished online: March 6th 2013. DOI: <10.3389/fmicb.2013.00015>.
Galán, J. C.; González-Candelas, F.; Rolain, J. M. and R. Cantón, 2013. «Antibiotics as Selectors and Accelerators of Diversity in the Mechanisms of Resistance: from the Resistome to Genetic Plasticity in the β-lactamases World». Frontiers in Antimicrobials, Resistance and Chemotherapy. Published online: February 8th 2013. DOI: <10.3389/fmicb.2013.00009>.
Levy, S. B., 2002. The Antibiotic Paradox. Da Capo Press. Cambridge, MA.
Linares, J. F.; Gustafsson, I.; Baquero, F. and J. L. Martínez, 2006. «Antibiotics as Intermicrobial Signaling Agents Instead of Weapons». PNAS, 103(51): 19.484-19.489. DOI: <10.1073/pnas.0608949103>.