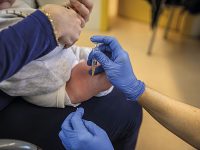
Pain is a subjective sensation, so to objectify its intensity different types of scales are used whereby the patient can indicate the degree of pain being treated. The effect of analgesic drugs is evaluated in clinical trials subject to strict rules in order to compare the effect of the medication with that produced by substances without analgesic activity.
We assume that the sensation of pain is subjective and therefore the only person capable of knowing the pain one suffers is the individual oneself. However, in order to treat pain we need to evaluate it objectively, so we can tell society, sufferers and specialists what medicine can be administered or the best way to combat pain.
Objective evaluation of pain itself
Of course, the extent and quality of the damage determines the pain, but this is modulated by the individual’s previous experience of pain and his emotional state at the time, hence the need to assess each case. Health professionals tend to underestimate their patients’ pain and to avoid this problem, tools are available which help record the painful experience reported by the patient in the most objective way possible.
Tools have been developed dealing with different aspects of pain that are not independent and are therefore difficult to separate. We might say that the questions to answer are: how much does it hurt? And how much am I suffering?
To answer «how much does it hurt?» or, in other words, to measure the intensity of pain, scales have traditionally been used to record the patient’s statement about the amount of pain experienced: the visual analogue scale, the verbal numeric scale and the verbal ordinal or categorical scale.
«We assume that the sensation of pain is subjective and therefore the only person capable of knowing the pain one suffers is the individual oneself. However, in order to treat pain we need to evaluate it objectively»
In the verbal ordinal scale, the patient selects the degree of pain from a number of categories offered. The oldest has four degrees of pain: none, mild, moderate and severe. These four levels may easily fall short in relation to the patients’ needs to express their pain and also some patients say that the difference between mild and moderate is less than between moderate and severe. Therefore other similar scales have been used with more categories to choose from, such as the 5-point scale (no pain, mild pain, moderate pain, severe pain, the worst pain imaginable) or the 8-point scale (no pain, barely noticeable, very mild, mild, moderate, severe, very severe, unbearable).
One way of avoiding misinterpretation of the terms that define the degree of pain and equalise the steps between the different categories is to use a rating-based scale. The most widely used involves asking the patient to rate his degree of pain from 0 to 10, the extremes being no pain and maximum pain. This numerical scale is easy to interpret and to use.
Generally, to apply the verbal scales little explanation by the assessor is needed, so no specialised training is required of the person collecting the data, which can be recorded by the patient’s family members or carers. It can also be collected via telephone or using other remote media. These features are advantages, but on the other hand, hearing and speech difficulties may be a problem.
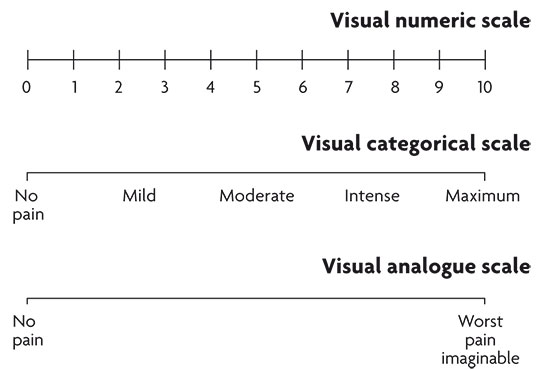
Different models of visual scales that help to measure pain intensity.
The visual analogue scale consists of a horizontal line, usually 10 cm in length, one end of which is «no pain» and the opposite end «the worst pain imaginable». The patient is asked to mark the line at the point which he believes represents his pain. The distance between the patient’s mark and the «no pain» end represents the intensity of pain in that individual. This type of scale can also be used to assess the emotional component of pain, i.e., the degree of suffering or other emotions that can accompany pain, such as anxiety, nervousness, etc… It may also be useful to determine changes in function of the affected organ.
The simplicity of this scale makes it one of the most used, although elderly patients or those with limited intellectual capacity may have difficulty understanding its meaning and operation. To make it easier there are line divisions, numbered from 0 to 10; the visual analogue scale becomes a visual numeric scale. Sometimes the line is not represented by division marks but a legend is added below on the degree of pain (mild, moderate and severe).
So we have seen how to transform verbal scales into visual scales. Also the verbal ordinal scale can be presented visually, using a written list of the various categories. In short, the aim is to adapt the question of interest «How much does it hurt?» to the patients’ capabilities. In this regard, as special cases, one must consider the situation of young children, the elderly and the disabled. Depending on the cognitive ability or the child’s age, different tools have been developed.
One of the best known is the graphic facial scale that can be used in children over three years old. It corresponds to the verbal ordinal scale for adults and, although it was introduced for children who are still not able to read, it can also be used in elderly patients or cognitively impaired patients.

Pain rating can present interpretation problems depending on patient characteristics. These difficulties are solved through physician-patient dialogue and consensus of experts in cases of patient groups. / © BananaStock Ltd.
In any case, the assessment of pain in patients with severe communication problems –whether due to age, condition, disability or mental illness– has a significant impact on these segments of the population. They are historically patients whose pain is hardly treated, because, according to the definition of pain provided by the International Association for the Study of Pain (IASP) and as described by Professor Baños, «pain exists when so declared by the sufferer… In other words, pain is present when the patient reports it and not when others believe it to be present. Such consideration would lead to a logical conclusion: who fails to report pain, does not suffer any such pain».
It is therefore necessary that those taking care of the patients or health care professionals assisting them should actively seek behavioural changes (restlessness, nervousness, sleep disturbances, etc..), changes in their vital signs (respiration, blood pressure) or other signs such as body position or facial expression that may be due to pain and thus may serve to diagnose, assess and treat it.
Different scales have been developed that take into account these expressions of pain, such as «Comfort» to evaluate children in intensive care units (ICU), which consider the muscle tone, body movements, facial expression and vital signs, such as blood pressure and heartbeat. Or the «Behavioural Pain Scale», which is also used for adult patients in the ICU and which uses four different points for each of the following three domains: facial expression, upper-limb movement and respiratory management.
«The assessment of pain in patients with severe communication problems –whether due to age, condition, disability or mental illness– has a significant impact on these segments of the population»
In any case, as noted herein, if it is not easy to standardise the process for measuring pain in people able to communicate, it is much more difficult when communication is limited. This situation requires more effort in research to determine the appropriate method for assessing pain in these circumstances.
As noted initially, pain assessment also involves characterising the associated suffering including disability and vital condition. We can use the same type of verbal or analogue scales defined for intensity but applied to measure limitations in everyday, social or work activities affected by the pain and «how the person feels», i.e., if he feels happy or sad, down or very energetic, whether he is in pain or not; ultimately the answer to «how much am I suffering?».
When the pain never stops
The quality rating of a painful experience acquires special significance in chronic pain, which is interpreted as a disease in itself, unlike acute pain, generally regarded as a symptom of an injury or illness.
Chronic pain, according to the IASP definition, is «that which exceeds the normal healing period». The patient perceives this as an unpleasant experience that does not serve to warn against damage, and easily leads to despair, with behavioural changes, isolation and affecting the individual’s social, family and working life. Therefore, to properly address it, one must assess it in all its dimensions.
Among pain-rating tools from a multidimensional perspective, one of the most recognised and used is the McGill Pain Questionnaire. It is a self-administered questionnaire, i.e., it does not need a survey taker, and has been translated into Castilian for the evaluation of Spanish patients. In its complete version, proposed by Melzack (1975), it comprises 78 adjectives divided into twenty groups.
Generally an abridged version is used which includes 62 different aspects (descriptors) that are distributed in fifteen sections, which in turn are classified into three types depending on the specific dimension evaluated (sensory, affective and evaluative or temporary). It also has a visual analogue scale for pain intensity, a categorical scale and a drawing of the human form on which one should mark exactly where the pain is located. Each category is assigned a score that gives a value to each of the dimensions and by adding these partial scores, we obtain a final numerical value called «pain rating index» (PRI).
For a full rating of the patient with pain, the McGill Pain Questionnaire includes personal data, a clinical record of the pain, the condition of the individual at the time of the interview, the influence of pain on daily life, previous and current pain treatments, health habits, and the patient’s social-family situation.
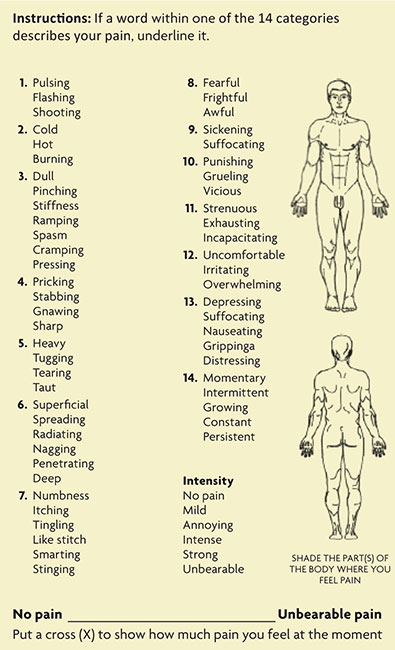
The McGill pain questionnaire can be completed by the patient, so that he himself rates his pain following a checklist.
Treatment effectiveness
Pain assessment can be performed as a standard medical measure in one patient alone or as part of a research studying the effect of treatment. In both cases it is interesting to know the outcome of the treatment, that is, if the pain has decreased and to what extent. To assess the degree of relief we can measure the intensity of pain after treatment and the difference with respect to that initially reported by the patient will give us information of the effect. It is also possible to directly question the patient about the degree of relief offering him preset categories (no pain relief, mild relief, moderate relief and complete relief) or numbers (from 1 to 10) so he may choose his condition.
It has been found that measurements repeated before and after treatment are less sensitive to assess the effect of treatment. In this respect, a study researching the analgesic effect in 1,500 patients concluded that the categorical scale of relief was the most sensitive for effect detection, followed by the visual analogue scale and categorical scale of pain intensity. These results were obtained after analysis of twenty clinical trials in patients treated with pain medication or placebo and, despite the differences between the scales rating the effect of treatment, 17 studies had reached the same conclusion regardless of the scale used.
In the previous paragraph we mentioned the method par excellence for evaluating the effectiveness of treatments used, not only for pain, but for any disease. It concerns clinical trials, comparing the drug with placebo. Clinical trials could be defined as an experiment planned to evaluate the effect of medicines on people who voluntarily, and after being thoroughly informed, consent to participate.
Put simply, placebo can be defined as a substance that looks like the drug but has no pharmacological activity, but may produce an effect based on the patient’s belief that he is taking something to cure himself or to alleviate the pain. The use of placebo is necessary to test the effect of a drug, because otherwise medicines could be marketed whose effect is equal to drinking a glass of water while affirming that the medicine is a cure.
In studies with analgesics, so as not to deprive the patient in the group receiving placebo of an effective pain treatment (random allocation is required), he will be given the so-called «rescue medication». Patients are told that if, after a reasonable time after taking the medication, there has been no analgesic effect they may take another medicine previously selected by the researchers. This procedure avoids the volunteer suffering unnecessarily, either because he is in the group taking placebo or because the drug under study does not have sufficient analgesic effect.
«The patient perceives this as an unpleasant experience that does not serve to warn against damage, and easily leads to despair»
In clinical trials of new analgesics, the placebo is used in short studies and generally in the early stages of research, for example to determine the dose to be chosen.
It seems reasonable to believe that the greater the need of rescue medication, the less the analgesic effect of the drug, so rescue medication is also used to measure the effect of the painkiller. For this method to be truly useful and not prone to errors, it must be very clearly expressed how the rescue analgesic will be administered, because as we have said before, if left to the opinion of health personnel, they will tend to underdose.
In order to assess the possible effect of a new drug on pain, not only do we have to select a sensitive and reproducible tool to measure pain, but also a suitable painful experience on which to apply it. That means selecting the painful stimulus, the disease that causes pain.
The method par excellence for evaluating the effectiveness of the treatment of pain or any disease is the clinical trial comparing the drug with placebo. / © BananaStock Ltd.
Studies on acute pain usually refer to postoperative pain in patients not only having the same type of surgery (on the chest, urinary tract, etc…), but also when the same surgical technique is applied. In this sense, an extraction of the third molar (known as wisdom tooth) is a widely used surgical procedure as a method of rating analgesics for acute pain. It has the advantage of being a standardised surgical technique and above all it is usually performed on young and healthy individuals, with no other health problems that hinder the interpretation of results.
This model highlighted the importance of the intensity of pain before administering the drug or placebo. Logically, if we act on a minor pain it is likely that both the placebo and the analgesic will reduce pain to almost zero, so we would not observe differences in the outcome for each of the groups and would have to conclude that the painkiller is not really such, as it has the same effect as placebo. It would also be very difficult in a study of mild pain to note the difference between a potent analgesic such as morphine and one not so strong, such as paracetamol. Both would relieve the pain and therefore we may conclude that they are the same.
The situations discussed have led us to recommend that studies to test the effectiveness of an analgesic should be conducted on patients with moderate to severe pain. In the case of pain resulting from a third molar extraction, 60% of patients report moderate pain and the others say pain is intense. Noteworthy is the importance of proper planning of the rescue analgesic, when we are talking about moderate to severe pain and patients treated with placebo.
«In clinical trials of new analgesics, the placebo is used in short studies and generally in the early stages of research, for example to determine the dose to be chosen»
To evaluate the effect of an analgesic in cases of chronic pain, there is no particular experimental model, partly because there are very different diseases that cause chronic pain and they respond differently to analgesics. Examples are migraine, cancer pain or pain in rheumatic diseases. So if we wish to research a new drug for chronic pain, we must select the disease on which to test its effect and the fact that a drug may be effective in a case of osteoarthritis, does not mean that it is for migraine. If it is to be prescribed for the latter, effectiveness against it should be proved
In studies of analgesia for chronic pain, the effect of the drug must be evaluated at various times throughout the study and it should be clearly specified when and how this is to be done. For this purpose the so-called «patient diaries» are used, which record data on the patient’s pain as scheduled and which will serve to test the effect of the drug under study. The patient’s memory cannot be relied on to describe their pain, because, as mentioned, former painful experiences modulate current pain. In fact it has been found that if the pain is intense at one point, the patient recalls pain experienced in past episodes as more intense than it actually was and vice versa.
In short, the evaluation of pain and its treatment presents difficulties that can be solved by dialogue between doctor and patient in order to treat the individual and by expert consensus when referring to studies1 on groups of patients.
NOTES
1. A good example can be found in papers published on the website IMMPACT group, acronym of «Initiative on Methods, Measurement, and Pain Assessment in Clinical Trials». (Back to text)
BIBLIOGRAPHY
Averbuch, M. & M. Katzper, 2000. «Baseline Pain and Response to Analgesic Medications in the Postsurgery Dental Pain Model». The Journal of Clinical Pharmacology, 40: 133-137.
Baños Díez, J. E., 2004. «Medición del dolor y el sufrimiento en personas con déficit de comunicación: Niños preverbales, ancianos con demencia y personas mentalmente discapacitadas». Monografías Humanitas, 2: 39-52.
Franck, L. S. & E. Bruce, 2009. «Putting Pain Assessment into Practice: Why Is it so Painful?». Pain Research & Management, 14: 13-20.
García-Alonso, F. et al., 1997. «El placebo en ensayos clínicos con medicamentos». Medicina Clínica, 109: 797-801.
Lázaro, C. et al., 1994. «The Development of a Spanish Questionnaire for Assessing Pain: Preliminary Data Concerning Reliability and Validity». European Journal of Psychological Assessment, 10: 145-151.
Ruiz-López, R. et al., 2011. «Medidas de dolor. Cuestionario del Dolor en Español (Mc Gill Pain Questionnaire-MPQ-; Melzack, 1975)». In Badia, X. (ed.). La medida de la salud: guía de escalas de medición en español. PPU. Barcelona.