 Aki Hänninen / SINC Aki Hänninen / SINC |
||
|
At the end of May, alarms went off: one boy in Olot was diagnosed with diphtheria. It is the first Spanish case in 28 years and the first in Catalonia in 32 years. «Currently it is an endemic disease in some regions of the world where vaccination coverage is under 50%. But there are no cases, or very exceptional ones, in countries where vaccination coverage reaches 90% in children and 75% in adults», explains Alma Bracho, member of the area of Genomics and Health of the Foundation for the promotion of Healthcare and Biomedical Research of the region of Valencia (FISABIO). Then, why has a disease that was believed to be eradicated in most of the world made a comeback in Spain? The answer is simple, «diphtheria has reappeared because bacteria found one specimen, or more, who was susceptible to contagion», she claims. The individual, a six-year-old boy, was not vaccinated against the disease. Diphtheria, a nineteenth century pandemic Before vaccination, diphtheria was a pandemic. According to María José Báguena, PhD in Medicine and Professor of History of Science at the University of Valencia, despite the fact that we do not know exactly when it started affecting people, descriptions matching diphtheria in ancient Greece have been found. Until well into the nineteenth century, it was not possible to distinguish different pathologies that obstructed the upper respiratory tract. «They were all grouped in Spanish as garrotillo, because the death by suffocation they produced was very similar to the kind of suffocation caused by garrote vil in executions», explains María José Báguena. In the nineteenth century, diphtheria, also known as croup, substituted smallpox as the main cause of infant mortality, especially among 2-to-6-year-old children. In Spain, at the end of that century, the infant mortality rate related to diphtheria was 0.66 cases every thousand inhabitants. It amounted to 2.51% of total deaths. The quest for the vaccine María José Báguena guides us from the beginning of the disease up to 1987, when the last diphtheria case was diagnosed in Spain: «In 1826, the French physician Pierre Bretonnau described the clinical characteristics of the disease for the first time and named it diphtheria. In 1833, Edwin Klebs isolated the responsible microorganism and, the following year, Friedrich Löffler managed to culture and reproduce the disease. The discovery of the toxin that caused the pathogenic action was made by Pierre Roux and Alexandre Yersin between 1888 and 1890». Then came the quest for a vaccine, which took its first steps when Émile Behring and Shibasaburo Kitasato identified the antitoxin that neutralised the effects of the toxin. «In 1893, Behring used this discovery to prepare a serum from immunised animals to treat the disease. Roux modified the serum and applied it successfully in 1894, producing a drastic decrease in the number of deaths related to the infection», says María José Báguena. The anti-diphtheria vaccine was discovered in 1923 and was introduced in the Spanish vaccination schedule in 1945, although the coverage was low. In 1965, however, the DTP vaccine was introduced (against diphtheria, tetanus and whooping cough). Now, three doses are provided during the first year, with three revaccinations at 18 months, 6 years and 14. The best prevention strategy Correct vaccination during early childhood for the majority of the population (between 90% and 95%) is precisely the reason why there had not been any new cases in Spain since 1987. Alma Bracho defends that vaccination «is the most effective strategy to prevent disease». Vaccination with diphtheria toxoid, which is the diphtheria toxin modified so that it loses its toxicity but keeps its immune response, provides immunity against the diphtheria toxin». And, while there is no diphtheria in most European countries, some cases have been described in Latvia, Russia and Ukraine. Furthermore, diphtheria is still endemic in many regions of the world, especially in certain areas of Latin America, the Caribbean, South-East Asia, Middle East and Africa. «As the possibility to be in contact with an imported case exists, the best prevention to control diphtheria is to maintain a high vaccination coverage», states Alma Bracho. However, the vaccine is very effective in the prevention of the most serious form of the disease and of mortality, but it does not protect against nasopharyngeal colonisation. This explains the fact that Corynebacterium diphtheriae bacteria have been found in eight vaccinated children who had been in contact with the child who is now in hospital, but do not show symptoms of the disease. The diphtheria routes of infection The main route of infection of diphtheria is through air, via direct physical contact with a patient or through an asymptomatic carrier, that is, people whose nose or throat is infected with Corynebacterium dipththeriae but do not show any symptoms. Corynebacterium diphtheriae, and sometimes Corynebacterium ulcerans or Corynebacterium pseudotuberculosis, are the causes for diphtheria, an acute bacterial disease that affects mainly the upper respiratory tract, nasal mucosa, tonsils, larynx or pharynx. The disease starts due to strains of toxic Corynebacterium, which produce the toxin. For a strain to produce toxin, the Corynebacterium bacteria must be infected with a bacteriophage, a virus that infects bacteria, with the gene of the diphtheria toxin. How to fight the disease «In order to eliminate the bacteria, a proper antibiotic treatment is enough. But to fight the produced toxin, diphtheria antitoxin must be administered. The success of the treatment depends on the speed with which the antitoxin reaches the patient. This medication neutralises only the circulating toxin, not the amount that has already affected the tissue. The lethality and associated complications are directly related to the time between the first symptoms appear and the administration of the toxin», explains Alma Bracho. In addition, one of the protocol actions is administrating prophylaxis to those who were in contact with a patient. Therefore, «vaccinating people susceptible to infection is one of the control measures that are being carried out from the Public Health Agency of Catalonia», she adds. So the possibility of new diphtheria cases has significantly been reduced. As previously mentioned, the probability will be lower the higher the vaccination coverage of the population. In this sense, Alma Bracho says that «epidemiologists speak about group immunity, which is generated by vaccinated people and prevents an infectious agent from spreading, because it does not find people susceptible to infection. Group immunity usually protects unvaccinated people, too, whether they decided not to get their inoculation or if it posed a risk to their health». Science, anti-vaccinationists and the media The fact that the parents of the child diagnosed with diphtheria decided not to vaccinate him brought the debate on vaccines to the covers of the newspapers, with experts defending vaccines and people questioning or opposing them. Many practitioners, however, denounce that the media gives a voice to the antivaccination movement. So did paediatrician Carlos González, interviewed by Antonio Martínez Ron: «most of the media who interviewed me recently, for instance, wanted to interview me, but also someone who was against vaccines, so they could have both options. You would never interview someone for and someone against drinking alcohol during pregnancy so you could show both options. Some things are simply nonsense, they are not even worthy of the name controversy». Alma Bracho shared his view: «I am against information being given in the form of a confrontation, where the advocate and the detactor of vaccines are put at the same level. The quantity and quality of the scientific evidence provided by an advocate for vaccination does not have a comparable counterpart. On the other hand, I find it surprising that some people or collectives who react against vaccines have a high level of education and consider themselves to be well informed. They show arrogance in front of professionals who understand disease prevention as far as scientific evidence allows. It is ultimately a matter of trusting or questioning the evidence provided by scientific research». As Núria Jar wrote in Mèdia.cat, «vaccines emerge from research, from the scientific method. Conversely, antivaccination arguments are constructed on ideology». Given the devastating impact of the lack of vaccination, which can bring back diseases that were considered eradicated in our country, we asked Alma Bracho how she would answer to an antivaccination message: «I would simply say that vaccines protect us from serious consequences of infectious diseases and from premature death, whereas non-vaccines do not. Vaccines are not exempt from side effects, as any other medication or treatment, but there are a lot of security controls in place, and the individual and group benefit from protection is far superior to the sum of all the possible side effects». She concludes, joking, «I prefer it when a product has small unwanted side effects. If it does not have any side effects, I start considering if it has any primary effects». Íngrid Lafita. Journalist. Mètode, University of Valencia. |
«In the nineteenth century, diphtheria, also known as croup, substituted smallpox as the main cause of infant mortality, especially among 2-to-6-year-old children»
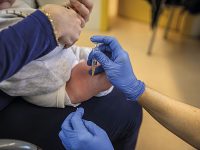
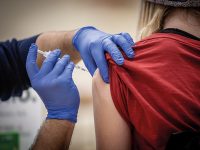
«As the possibility to be in contact with an imported case exists, the best prevention to control diphtheria is to maintain a high vaccination coverage» «One of the protocol actions is administrating prophylaxis to those who were in contact with a patient» «The quantity and quality of the scientific evidence provided by an advocate for vaccination does not have a comparable counterpart» |
|