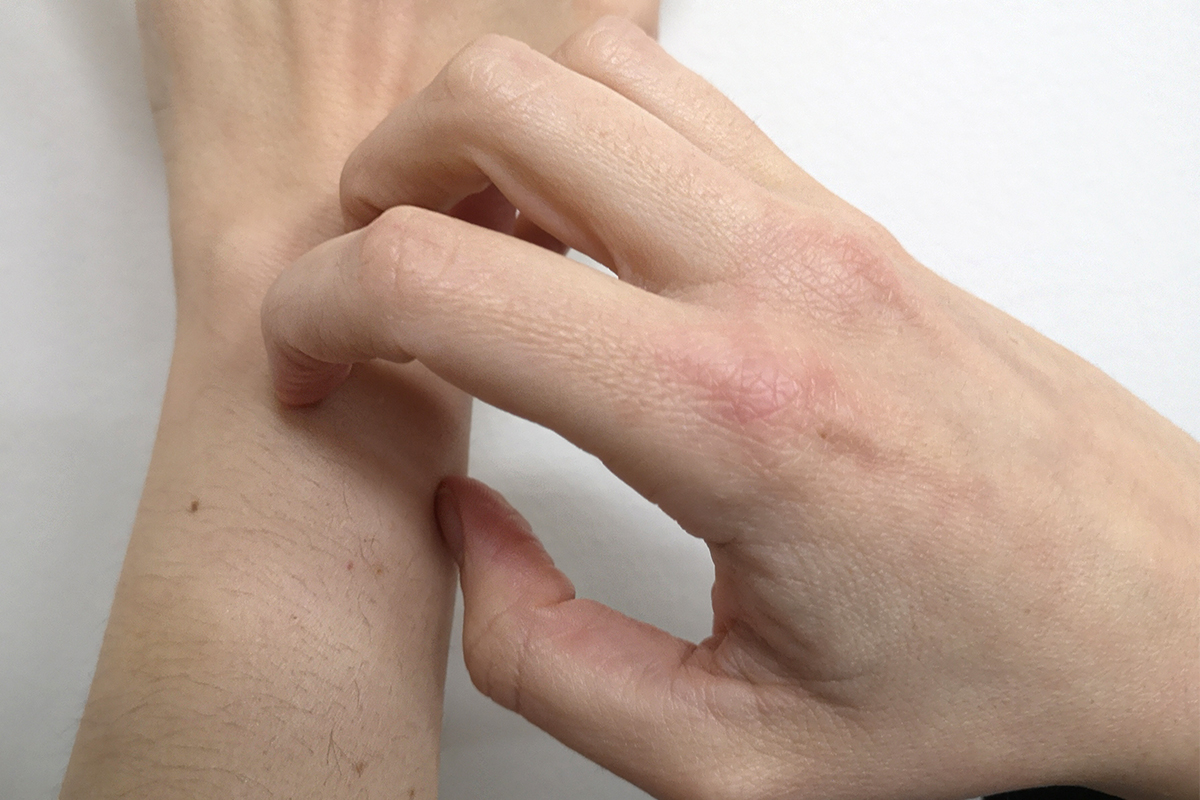
The last decade has seen a marked increase in the incidence of scabies in Spain, although the reasons that may have contributed to this are not yet clear. The COVID-19 pandemic has made the situation even worse and dermatologists report many more cases than before the health crisis. It is difficult to know the full extent of this increase in scabies cases, because reporting cases of the disease is not mandatory.
Health officials are considering several factors that might be responsible for the increased frequency of this infectious skin disease caused by the Sarcoptes scabiei mite. It seems likely that confinements, especially the one that took place in March 2020 and lasted several months throughout the country, led to the spread of this arachnid, as a result of much closer contact in households. In addition, the saturation of health services and the fear of going to the doctor because of the risk of SARS-CoV-2 infection delayed timely treatment to eliminate the parasite, thus increasing the likelihood of contagion from affected patients.
The mite responsible for scabies usually requires direct skin-to-skin contact between people for transmission, and so overcrowding is a risk factor. However, infection through clothing, bedding, etc. is also possible. Transmission in fitting rooms is not impossible, but very unlikely, due to the limited time of exposure and because the parasite can only survive for 2–4 days outside the human body and is usually nocturnal.
Scabies may seem like a disease of centuries past, but it is still very much present in the poorest parts of the world, where up to 10% of children may suffer from it. According to the World Health Organization, around 200 million people suffer from scabies. They are mainly concentrated in hot tropical countries and densely populated areas.
The skin-burrowing mite
Scabies is a familiar old human disease. Its most representative symptom is an intense itching, which predominates at night. The first references to the disease date back to 482 BCE in ancient Egypt, although it certainly affected people much earlier. Illustrious figures such as Aristotle once documented the presence of «lice» emerging from certain skin lesions. However, many centuries would pass before the cause of scabies became completely clear. It was not until 1687 that the physician Giovanni Cosimo Bonomo first identified the perpetrator thanks to the invention of the microscope: the Sarcoptes scabiei mite. However, the blame on this tiny arachnid was shrouded in scientific controversy and it was not until 1834 that its existence was fully accepted in the medical community.
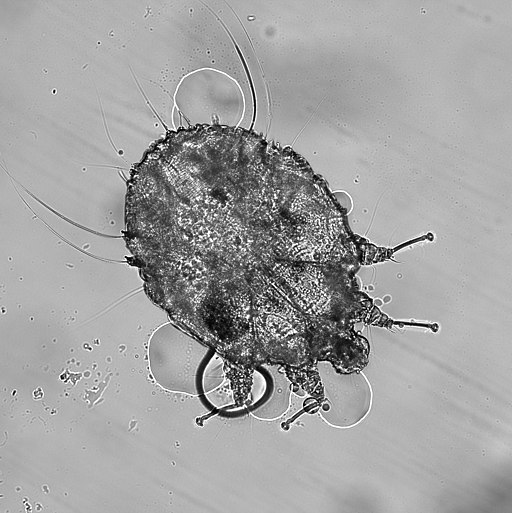
Detail of a Sarcoptes scabiei seen under an optical microscope. / Photo: Arthur Goldstein, CC BY-SA 4.0, via Wikimedia Commons
Unlike other mites that live with humans and are generally harmless (except for potential allergies), such as dust mites or Demodex mites, Sarcoptes scabiei var. hominis is an obligate parasite that causes characteristic skin lesions throughout its life cycle. They have four pairs of legs (in the adult stage), are round, whitish, and spiny animals that specialise in parasitising only humans, the only environment in which they can complete their life cycle.
Females (300–450 microns) and males (150–250 microns) copulate in small creases in the surface of the skin and, after this stage, the males die and the females burrow into the outermost layer of the skin (the stratum corneum) to create tunnels about 1–10 mm long. The females lay eggs (30–50) in these tiny grooves for 4–6 weeks, and they die after the process is complete. The eggs hatch in just 3–4 days as larvae, pass through the nymph stage, and reach the adult stage in 12–15 days.
In general, a typical infection usually involves around 10–15 female burrowing mites. However, immunocompromised people can suffer from a massive infestation of burrowing mites called Norwegian (or crusted) scabies, with thousands or millions of burrowing mites and little or no itching at all (due to minimal immune response). This form of the disease is serious, with potential complications such as life-threatening infections. In addition, the patient is highly contagious due to the high number of Sarcoptes present on the skin.
The scabies mite has a preference for areas with creases such as the spaces between the fingers, wrists, elbows, armpits, the area around the navel, buttocks… The itching and rashes are not provoked by the direct damage caused by the tiny mites, but by the inflammatory reaction triggered by the presence of faeces and proteins of this arachnid inside the burrows. For this reason, people who are infected for the first time may take 5 to 15 days to develop the characteristic itching (some may take up to a month), as this is the time it takes for the immune response to develop. However, people who have been infected before experience symptoms just 1–4 days after infection, with a much earlier inflammatory reaction.
Fortunately, drug treatments, if applied correctly (to all infected people living together) and for a sufficient period of time, are very effective against these parasites. Pharmacological options include permethrin 5% applied to the skin, oral ivermectin, and benzyl benzoate lotion 10–25%. Washing clothes, sheets, and towels with detergent at 60°C to destroy Sarcoptes is also essential to cut down the infection. Textiles that cannot be washed can be kept in hermetically sealed plastic bags for a minimum of four days to be sure that the mites are destroyed.





