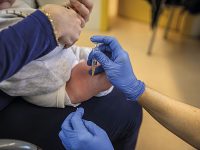
Children experience pain just like adults, since nerve pathways develop during pregnancy. Pain in infants has particular connotations because it is difficult to assess, but there are validated methods to detect it and, above all, there are procedures and medicines to treat pain effectively in children.
Why should we devote an article to pain in children? Does this context differ from adults? Based on the definition of pain as an unpleasant sensory and emotional experience, it seems logical that children are equally prone to suffering it as adults. For many years we were under the misconception that children had a lower perception of pain due to the immaturity of their nervous system. Nothing is further from the truth. Indeed, it has been shown that between the second and third trimesters of pregnancy the neural pathways for pain develop.
What is true about pain in children is that it has special connotations, on the one hand due to the difficulty children have in understanding what it is and in expressing themselves and, on the other, the difficulty adults have in interpreting and, therefore, preventing or treating pain.
«Pain in children has special connotations due to the difficulty children have in understanding what it is and in expressing themselves, and the difficulty adults have in interpreting them»
Painful experiences in childhood, even when they are not remembered, will change the child’s perception and attitude to pain later in life. Studies of preterm infants that undergo extensive testing or painful techniques (multiple blood extractions, intubation…) from birth indicate they have a lower tolerance to pain and are more fearful of potentially painful situations in later life. It has been demonstrated that children who suffer from pain in neonatal units fare worse because they have lower oxygen concentration, increased cardiovascular instability and higher intracranial pressure; moreover, their neurological development is slower. For all these reasons, it is especially important to recognise and avoid unnecessary pain in children, pain that can and should be avoided with the proper treatment.
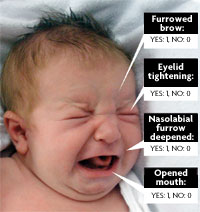
The facial expression of young children (under three) can help us to assess pain. If the various elements shown in the image are present, they are scored 1 or 0, which allows us to compare the situation before and after treatment. / © Mètode
Understanding pain in children
Assessing pain in children is a difficult task, since it is a symptom and is, therefore, subjective. To this we must add the fact that how pain is perceived, interpreted, lived and, above all, expressed varies depending on the patient’s age. Children under two have no concept of time, and have difficulty understanding pain: what is it and how long it will last. Therefore pain is invasive and it scares them. From two to seven years of age, kids have an egocentric view of the world, they believe someone is responsible for their pain but do not know how to locate it. Seven to eleven year olds have developed logical thought, so they can explain, locate and quantify the intensity of pain. And finally, over elevens can understand that they can do something to modulate pain, and so they need information about pain and how to treat it. All these aspects must be taken into account when assessing and treating pain in children.
Despite the difficulties in assessing pain in children, there are numerous approved methods and scales enabling objective measurement. To assess pain in children under three years of age, signs derived from their stress response can help us, such as heart rate, breathing, high blood pressure or sweaty palms. There are other behavioural signs such as facial expressions, screaming, crying and body movements (withdrawal reflexes). One should not always expect crying or irritability, especially in cases of chronic pain, in which children may express their pain through excessive stillness and calm.
In children over six years of age, visual analogue scales can be used, similar to those used for adults. In the most commonly used model respondents specify their level of agreement to a statement by indicating a position along a continuous line between two end-points representing «no pain» or «excruciating pain». However, for children graphic scales may be more useful, with facial drawings expressing varying degrees of pain, or colour, numerical or verbal scales.
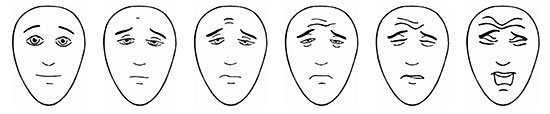
Spafford’s graphic scale is a paediatric tool used to assess pain in children. Pain intensity is measured as 0, 2, 4, 6, 8 or 10 according to the face chosen. / © IASP
Spafford’s Faces Pain Scale consists of six faces with different expressions and is internationally recognised for pain assessment in children with instructions for use in numerous languages, including Spanish and Catalan. Children are told that the face on the left shows someone who has no pain and the children on the right feel increasingly intense pain, ending up with excruciating pain on the far right. They are then asked which one is most like their own pain. As in adults, such scales should be used to assess the initial pain and then after treatment to assess its efficacy.
Pain relief in children
There are pharmacological methods to treat pain in children, which are particular to paediatrics, and non-pharmacological methods, whose purpose is to lessen pain and boost the sick child’s own health resources. The latter should always be used, even in conjunction with drug therapy, the most common being:
Distraction. Diverting attention by using music, stories, videos, helping them think pleasant thoughts or doing things like blowing up balloons, counting backward, and so on.
Cutaneous stimulation. Massage, pressure with or without massage, applying heat or cold.
Relaxation. Children over three or four can be told to breathe slowly and deeply. Younger children can use a pacifier (with a few drops of glucose or saccharin, since several studies have shown this method to be effective).
Positive reinforcement. Increased self-esteem helps children to positively assess their ability to tolerate pain.

A non-pharmacological method used to relieve pain in children is distraction. This is done by diverting little ones’ attention through games, music or stories. This is why play parks and library services are often found in hospitals for younger patients, providing games or activities to distract them. / © De La Ribera University Hospital, Alzira
There is a lot of information about one particular non-pharmacological method, which concerns the use of oral sucrose. Studies show that children between two and four months of age given 0.6 ml/kg of 24% sucrose solution during immunisation experienced less pain than children of a similar age who were given water. Some paediatricians have proposed the systematic use of this procedure during the vaccination process.
Parents play an important role in implementing non-pharmacological methods to avoid unnecessary pain, and to help them in this task they should be properly informed by health professionals.
Analgesics are used to treat pain pharmacologically. Although there are many different drugs, few receive paediatric approval: acetaminophen, ibuprofen, metamizol and codeine. The latter, however, despite being a proven pain reliever can also be associated with acetaminophen, and is sold in Spain only as a cough medicine.
Until the eighties, aspirin was the analgesic of choice in paediatrics. However, it is currently contraindicated in patients under sixteen years of age because its use to treat fever in some viral infections, such as chickenpox, has been associated with a severe and potentially fatal condition called Reye syndrome. What is more, there are now alternatives with a better safety profile, such as acetaminophen or ibuprofen.
For most drugs used in paediatric medicine, clinical trials are not conducted using children and therefore the results must be extrapolated from trials in adults. This means that the dosage is calculated from the usual dose in adults, either in terms of weight or body surface area (BSA) or age range. Painkillers are no exception, and limited clinical research in children means the authorisation to use drugs in this age group and the conditions of use do not coincide in different countries. A recent Italian study shows that acetaminophen –among other drugs–, which is approved and widely used for children, has different usage conditions in Italy, France and the UK. In Italy, dosage is adjusted to the child’s weight while in the United Kingdom it goes by age group and in France by the two methods combined. What is remarkable is that the doses do not coincide. Does it make sense that a child of equal age and weight receives a different dose of acetaminophen based on that fact he/she is French, English or Italian? The public should not be alarmed, the differences may not be that important, but an effort should be made to harmonise the authorisation and conditions of use of different drugs in the international arena. In fact, the European Medicines Agency is promoting the study of drugs in children, including analgesics, and harmonisation of information and legal conditions of use.
Children can experience pain from the moment they are born and this is of importance as early painful experiences may influence later development. Therefore, it is necessary –as far as possible– to prevent and relieve pain in children, and parents can play a key role in this task.
European Medicines Agency. Paediatric Medicine Development. European Medicines Agency.
Hatfield, L. A. et al., 2008. «Analgesic Properties of Oral Sucrose During Routine Immunizations at 2 and 4 Months of Age». Pediatrics, 121: 327-334.
Hicks, C. L. et al., 2001. «The Faces Pain Scale-Revised: Toward a Common Metric in Pediatric Pain Measurement». Pain, 93: 173-183.
Narbona López, E. et al., 2008. «Manejo del dolor en el recién nacido». Protocolos de la Asociación Española de Pediatría.
Perquin, C. W. et al., 2000. «Pain in Children and Adolescents: a Common Experience». Pain, 87: 51-58.
The Children’s Hospital at Westmead & Sydney, 2010. Fact Sheet Children’s pain-the facts. The Children’s Hospital at Westmead & Sydney.